
Welcome To Family Eye Care Services
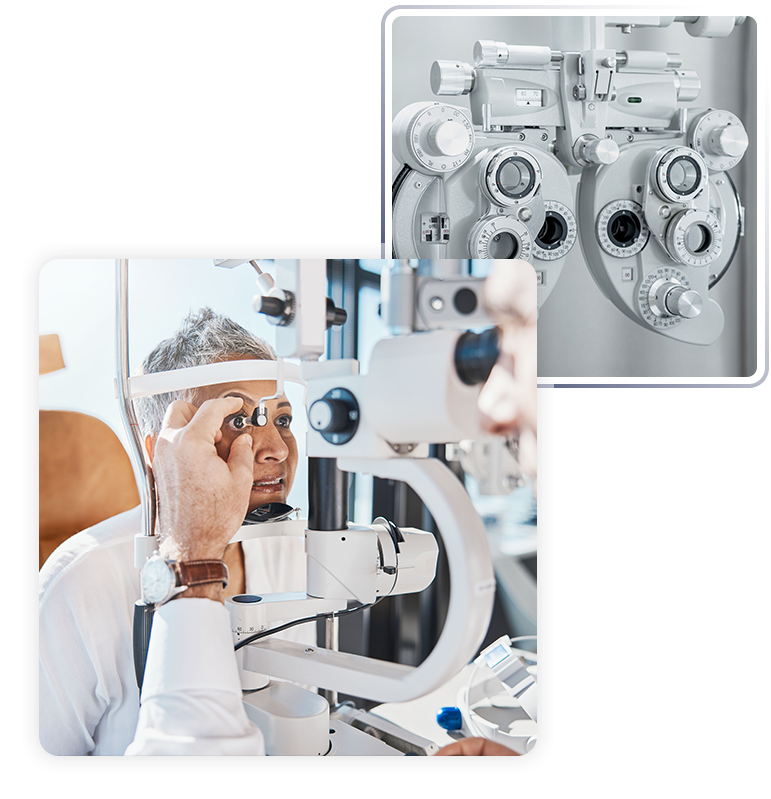
We are committed to providing outstanding eye care and the finest personal service in Bridgewater and Rockaway New Jersey. Our doctors are handpicked for their caring bedside manner, clinical expertise, and many years of experience.
We focus on diagnosing and treating eye conditions and diseases, fitting you with the right contact lenses for your needs and complete eye exams.


Dry Eye Relief with OptiLight & OptiLift
Find lasting comfort from dry, irritated eyes with our advanced light-based therapies. OptiLight and OptiLift target the root causes of dry eye, reduce inflammation, and restore healthy tear function so your eyes feel refreshed and hydrated again.
Learn More

Protect Your Child’s Sight for the Future
Nearsightedness often gets worse as kids grow. Our myopia management program uses advanced treatments like MiSight, ortho-k, and atropine therapy to slow progression and keep their vision clear and healthy.
Learn More































